Benign prostate hyperplasia (BPH) is the most common urological condition among elderly men, beginning around the age of 30 and reaching a prevalence of up to 90% in men in their 80s. It is a non-cancerous enlargement of the prostate which may develop gradually over a number of years. The gradual increase in size may be symptom free until it has enlarged sufficiently to press on the urethra and impede the flow of urine. Symptoms of increased urinary frequency, urgency, night-time urination, difficult and slow urination may be experienced as a result; they may be mild through to severe, impacting quality of life.
The prostate gland
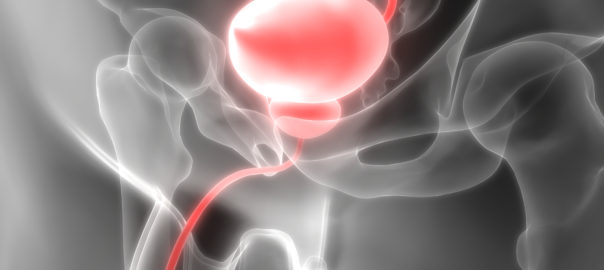
The prostate is a small gland found only in men. Initially the size of a walnut, it gets larger with age. The prostate surrounds the urethra just below the urinary bladder and is responsible for making the thick white fluid that mixes with sperm to create semen. It is surrounded by a layer of muscle and a fibrous capsule. In BPH the connective tissue (stromal) cells and epithelial cells proliferate excessively and this is coupled with reduced cell death.
Causes of benign prostate hyperplasia
A number of factors have been implicated in the aetiology of BPH including hormonal changes, oxidative stress, inflammation as well as ageing and metabolic syndrome.
Hormonal changes – In the prostate and other tissues, the male androgen testosterone is converted to dihydrotestosterone (DHT) by the intracellular enzyme 5-alpha reductase. DHT has growth promoting effects which in early life are responsible for the development of the prostate, penis and scrotum. In later years these effects can lead to prostatic hyperplasia. DHT is 10x more potent than testosterone and has been a target for drug therapy. To reduce the conversion of testosterone to DHT, men with BPH may be prescribed an inhibitor of the 5-alpha reductase enzyme. These drugs have been found to be effective in reducing prostate size and associated symptoms but have a number of adverse effects ranging from impotence to gynaecomastia (breast tissue enlargement).
It was thought that high levels of testosterone increased BPH and that testosterone replacement therapy therefore increased the risk, but this has not been supported by research and in fact low levels of testosterone (eg which occur in ageing) may increase the risk, possibly because testosterone has anti-inflammatory effects. In addition, there have now been a number of studies which show a link between low DHT levels and increased inflammation. Current thinking is that androgens have a role but other factors are necessary for the development of BPH.
Oestrogen may also play a role – the prostate is an oestrogen target tissue and ageing and obesity increase the plasma oestrogen to androgen ratio. Environmental oestrogens which are endocrine disruptors may also play a role – oestrogens in the water, plastics (eg BPA) etc. They are certainly having an effect on sperm counts and earlier this week it was reported that men’s sperm counts have halved in the last 40 years. On the other hand, dietary phyto-oestrogens may have a protective effect on the prostate, they are weakly oestrogenic and compete for oestrogen receptors thus blocking and reducing the more potent endogenous (internal) and exogenous (external) oestrogens from binding.
Oxidative Stress – has been considered to be one of the mechanisms that triggers the development and progression of BPH. Levels of antioxidants, including zinc, are decreased in prostatic hyperplasia. In addition, animal models with BPH have shown increased prostatic lipid peroxidation and reduced endogenous antioxidants (eg glutathione, superoxide dismutase and catalase).
Inflammation – Chronic inflammation is a common finding in BPH. A significant correlation has been found between prostate size and both acute and chronic inflammation and data suggest that this could be a causative effect, rather than occurring simply as a consequence. Potential causes include infectious agents, environmental factors (toxins), diet, lifestyle, hormonal or metabolic imbalances or a combination of these. Low testosterone is also associated with increased inflammatory mediators; and there have been a number of studies that show a link between decreased DHT levels and increased inflammation.
Nutritional support
Research has shown the prostate gland is one of the tissues where dietary polyphenols exert their actions and studies are reviewed in a paper by Elazu et al (2017). Polyphenols are plant based molecules with antioxidant properties. They may also have phyto-oestrogenic activity. They are classified into 5 groups including flavonoids (eg quercetin, rutin), curcuminoids (eg curcumin), phenolic acids (eg gallic acid), stilbenes (eg resveratrol), and lignans (eg beta-sitosterol).
The different polyphenols have been shown to exert one or more of a number of actions on prostate tissues including:
- decreasing growth factor expression
- inhibiting inflammatory mediators
- inhibiting 5-alpha reductase enzyme
- acting as selective androgen modulators ie decreasing DHT action;
- inducing cell death
- repairing antioxidant defence mechanisms (eg superoxide dismutase and glutathione peroxidase); and
- having phyto-oestrogenic activity
Foods rich in polyphenols include tomatoes, seeds (eg pumpkin, flax, sesame), nuts, green tea, cocoa, olives, parsley, celery, kale, broccoli, spinach, legumes and berries/grapes.
Tomatoes – are an excellent source of lycopene, a carotenoid responsible for its red colour. Lycopene is also found in a number of other foods including watermelon, pink grapefruit and guava. A beneficial role suggested for lycopene in patients diagnosed with BPH resulted in a pilot study of elderly men diagnosed with BPH. The effects of the intervention on carotenoid status, clinical diagnostic markers of prostate proliferation and symptoms of disease were assessed. Those taking lycopene had increased plasma concentrations of the carotenoid and showed no further enlargement of the prostate; in contrast progression of BPH continued in the placebo group. The researchers concluded that lycopene inhibited the progression of benign prostate enlargement.
Pumpkin seeds – contain a wide range of vitamins, minerals and amino acids and are a source of mono- and polyunsaturated fats. They are well known for their zinc content and men with prostate problems have been noted to have dramatically decreased zinc levels. Pumpkin seed has historically featured in the natural approach to treatment for BPH in a number of countries. Potential anti-androgen and anti-inflammatory properties were suggested as the benefit of the pumpkin seed to the prostate – research showing significant results achieved on the International Prostate Symptom Score (IPPS). Results showed IPPS score was reduced after 3 months of pumpkin seed supplementation, with the urinary flow rate showing improvement of statistical significance after six months.
Nuts – contain the plant sterol beta-sitosterol. The various plant sterols have shown a number of potential health benefits with beta-sitosterol demonstrating specific benefits in benign prostatic hyperplasia. A 1998 systematic review of 4 randomised controlled trials involving 519 men found that beta-sitosterol significantly reduced the International Prostate Symptom Score at 4 to 26 weeks.
If you have any questions regarding the topics that have been raised, or any other health matters please do contact me (Clare) by phone or email at any time.
clare@cytoplan.co.uk, 01684 310099
Clare Daley and the Cytoplan Editorial Team
Cytoplan products:
Prostate Support – Urtica Dioica, Beta-sitosterol, Pumpkin seed, Lycopene and Zinc in a wholefood base
Phytoshield – Mixed flavonoids and carotenoids in a brassica base
CytoRenew – Acetyl-L-Carnitine, Alpha Lipoic Acid, Ginkgo Biloba, CoQ10, N-Acetyl-L-Cysteine and Rosemary extract 5:1
Phyte Inflam – Curcumin from turmeric and gingerols from ginger root
Liposomal Glutathione – N-Acetyl L Carnitine, Alpha Lipoic Acid, Gingko Biloba, Rosemary Leaf Extract, Liposomal Glutathione and Resveratrol
CoQ10 Multi – CoQ10, Beta 1-3, 1-6 Glucan, vitamins B and D12, Acerola Cherry and carotenoids
Bibliography:
Elazu C, Elazu K and Kalu W (2017) – Management of benign prostatic hyperplasia: could dietary polyphenols be an alternative to existing therapies? Frontiers in Pharmacology, 8, 234
Hong H et al (2009) – Effects of pumpkin seed oil and saw palmetto oil in Korean men with symptomatic benign prostatic hyperplasia. Nutrition Research and Practice, 3, (4), 323-327
McNicholas T & Kirby R (2011) – Benign prostatic hyperplasia and male lower urinary tract symptoms (LUTS). BMJ Clin Evid, 1801
Nicholson T M & Ricke W A (2012) – Androgens and estrogens in benign prostatic hyperplasia: past, present and future. Differentiation, 82, 4-5, 184-199
Schwarz S et al (2008) – Lycopene inhibits disease progression in patients with benign prostate hyperplasia. J of Nutr, 138, 49-53
Unnikrishnan R et al (2017) – Benign prostatic hyperplasia: Evaluation and medical management in primary care. Cleveland Clinic Journal of Medicine, 84, 1, 53-63
Vignozzi L et al (2012) – Anti-inflammatory effect of androgen receptor activation in human benign prostatic hyperplasia cells. J Endocrinol, 214, 31-43
Yana M et ak (2010) – Differential response to zinc induced apoptosis in benign prostate hyperplasia and prostate cancer cells. J of Nutritional Biochemistry, Vol 21, 8, 687-694.
Last updated on 2nd August 2017 by cytoffice


Thank you for this excellent article with relevant supplements recommended for prostate support. I have a good ratio of male/female patients and most male patients have issues with frequency of urination, especially at night. Is there a reason why night time increases the frequency?
Dear Cynthia,
Thank you for your question. Yes, the frequency is increased at night time because lying down tends to put prostate and bladder in close contact and hence if prostate enlarged there will be pressure on the bladder. Plus any degree of hyperplasia is usually accompanied with inflammation – as bladder and prostate lie close together this will also affect bladder increasing tissue sensitivity within. But the main thing is, lying down increases intra-pelvic pressure.
All the best,
Amanda
Is there any ointment that can be used for treatment
Hi – While the supplement and dietary advice outlined in the blog can certainly support BPH, I’m afraid we don’t produce an ointment that would be suitable. I would recommend you spoke to your GP about possible treatment options.
How is it related to sexual activity
Sex drive may decrease as a side effect of medications used to treat BPH. However, symptoms related to BPH are complex and it is always best to consult with your doctor if you are experiencing BPH, especially in relation to sexual activity.
Very informative post! Can you please tell me about the foods that men should avoid or limit to prevent Benign Prostatic Hyperplasia?
Hi Alaina,
Thank you for your comment. The best foods to go for are unrefined, low glycaemic, and have high vegetable content. The paleolithic diet is a good diet to focus on – visit the following blog link for further information: https://blog.cytoplan.co.uk/microbial-translocation-lipopolysaccharide-key-mediator-disease/
As well as the nutrients listed in this blog, the diet that will help protect from prostate cancer is the same diet that will protect from most diseases – plus additional nutrients including selenium, zinc and lycopene.
Regards,
Amanda
Very informative and I really applaud it.
Very much informative and write up. Besides would like to suggest a medicine for BPH, I’m 54 years old having low urine flow, and may I upload my USG and how? Kindly help me out
Hello – We do a product called Prostate Support (2 per day). But if you would like more tailored support I suggest that you complete a health questionnaire – at this link.
Thanks,
Helen
Hi. I m 60 years. My prostate gland enlarged. .54 gram. I used capsule. Maxflow. D last three months and take relex
Hi Muhammad I’m afraid I don’t quite understand the question. If you haven’t already done so I would certainly recommend a visit to your GP to confirm a diagnosis of BPH. I would recommend you get in touch with our team of nutritional therapists on nutrition@cytoplan.co.uk who will be able to provide further support.
I am 55 year, my prostate have increased what I do now please help me
Hi Zahoor – Prostate enlargement is not uncommon in men over the age of 50 and most often not a serious problem.. Please visit your Doctor for an examination and the reassurances you seek as your Dr needs to be aware of tis. The nutrients that can help with prostate enlargement (hyperplasia) are zinc, selenium and lycopene. These are al in our Prostate support, or zinc and selenium are found in most multiformulae and lycopene can be obtained from tomatoes that are gently cooked in olive oil.
Can BPH be reversed and what drugs or supplements can be used?
Hi Bernard,
Thank you for your comment. To help us offer support safely and effectively, please complete our FREE health questionnaire (here).
Thanks,
Amanda
At what level or stage prostrate enlargement results to cancer?
Hi Daniel – Benign prostate hyperplasia is a non-cancerous enlargement of the prostate gland. If you would like to discuss your individual health concerns with one of our nutritional therapists, please email nutrition@cytoplan.co.uk
Can a benign enlargement of prosaic be reverse
Hi Arthur – In principle, benign prostate hyperplasia can be modified and reversed. It is important to identify what is causing the enlargement and from there it is normally wholly modifiable -although unless it is disruptive to daily life by increasing regularity of need to urinate, it does not present a health issue. A change in hormones as one ages can often be the cause of the problem..
Size of of BPH can be Decreased or not by medication ..
How to cure prostrate without operation????
Hi – The exact cause of benign prostate hyperplasia is unknown and there are likely to be several contributing factors such as hormonal changes, oxidative stress, inflammation and ageing. Dietary phenols; plant based molecules with antioxidant properties, that may also have phyto-oestrogenic properties have been shown to have a positive effect on the prostate tissue. Foods rich in polyphenols include tomatoes, seeds (eg pumpkin, flax, sesame), nuts, green tea, cocoa, olives, parsley, celery, kale, broccoli, spinach, legumes and berries/grapes so you could increase your dietary intake of these foods, or take specific supplements to support your prostate health.
I have 25.17 ml enlarge prostate.
Is it treatable and what precautions should I take
If you haven’t already done so I would certainly recommend a visit to your GP to confirm a diagnosis of BPH. I would recommend you get in touch with our team of nutritional therapists on nutrition@cytoplan.co.uk who will be able to provide further support.
Is it true that eccess acid in the body may cause prostate gland
Hi Kasyemo – The exact cause of benign prostate hyperplasia is unknown and there are likely to be several contributing factors such as hormonal changes, oxidative stress, inflammation and ageing. Dietary phenols; plant based molecules with antioxidant properties, that may also have phyto-oestrogenic properties have been shown to have a positive effect on the prostate tissue. Foods rich in polyphenols include tomatoes, seeds (eg pumpkin, flax, sesame), nuts, green tea, cocoa, olives, parsley, celery, kale, broccoli, spinach, legumes and berries/grapes so you could increase your dietary intake of these foods, or take specific supplements to support your prostate health.
Yes the comments are helpful but now it looks like theres no recommended treatment which has been tried found and recommended to be curing an enlarged prostate.
We would always recommend that you discussed your concerns with your GP in the first instance. There is a wealth of evidence to show that lifestyle changes, such as moderate exercise, diet modification, the intake of nutrients such as Vitamin D and Zinc as well as certain nutritional supplements can positively influence the symptoms of BHP.
Very nice and most informative
I am 62 urs.old.I have a problem for prostate enlargement.(BPH)since last six years.PSA test indicates
4.1.Is there any possibility of prostate cancer?
Hi there – this is not something we would be able to advise on I’m afraid, and we would recommend you visited your GP with your concerns.
Hi can someone be fertile again after removal of prostrate
Hi Andrew – as we are not medically trained, we would recommend you discussed your concerns with your GP or other medical professional.
The way this article was set is to go up and down including so many factors responsible of the enlargement of the prostate in a shambolic way. It is rather said that we do not know the real reason behind this enlargement and finish with it.
I beleive that sience should be humble enough to look for an old treatment in the ancient time rather than Confusing this issue further!
Nazar Zeki Mustafa
My psa is 9.37.I pee normally no oain.I take finca-5 once a day for the past 2 years.Take statin, carloc, pressure tablets.
Hi There – I would refer you to our most recent blog on the topic, which might help to answer your queries. Prostate health: nutrition and lifestyle interventions – Cytoplan
BPH can raise PSA, but we would always recommend that if your PSA levels are raised you consult with a medical professional.
Why psa high,is it?Any natural ways to bring psa to normal.
Hi There – if you wanted to send over a little more information to our team of Nutritional Therapsts, including a full list of your named medications, they will be able to help. nutrition@cytoplan.co.uk